We’ve created this article for National Pain Week 2020. Chronic pain is an issue that millions of people worldwide, and 1 in 5 Australians struggle with each day. Often these people are overlooked and misunderstood.
At honahlee, our goal is to help educate the cannabis community. It’s important that people understand pain and how it affects those around them. It’s also important for people to understand that a major treatment for chronic pain, opioids, is actually creating a whole new class of issues, and that cannabis can help treat chronic pain.
In this article you’ll learn about chronic pain and how medical cannabis for pay may reduce the need for opioids. Our goals for this article are:
- Raise awareness for chronic pain and people with chronic pain.
- To help explain the opioid crisis with relation to chronic pain.
- Explain opioid use disorder and how cannabis is helping to treat both opioid use disorder and chronic pain.
If you’d like to jump ahead in the article you can use this index:
- What is chronic pain?
- The impact of chronic pain in Australia.
- Pain treatments.
- The evolution of the opioid problem.
- Understanding opioid addiction.
- Opioid use disorder (OUD) and chronic pain treatment.
- How cannabis helps with OUD and chronic pain.
- Much needed changes.
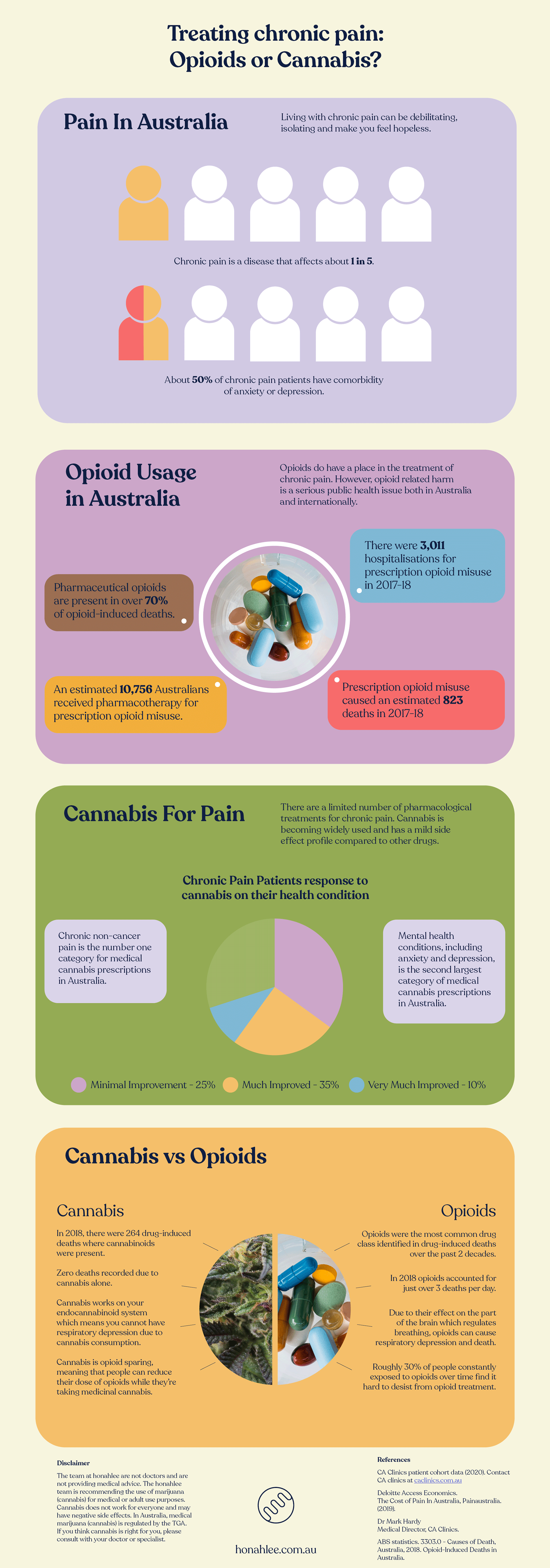
Or you can view the Treating Chronic Pain: Opioids or Cannabis infographic below.
Understanding Pain
Pain is an unpleasant, sensory and emotional experience associated with actual or potential tissue damage. There are three major categories of pain
- Acute pain
- Cancer pain
- Chronic pain
Pain is a sensation that we all experience. Feeling pain can be normal in some circumstances. However, if pain persists for a long period of time, it can be detrimental to your health.
What Is Chronic Pain?
Pain Australia defines Chronic pain as pain that has lasted beyond it’s expected treatable or healing time, usually more than three months. The term ‘chronic’ pain just means that the pain is persistent and doesn’t tell us about the quality of the pain.
Pain can be a symptom of a disease, for example pain as a result of cancer, or it can be a disease in itself. If you experience pain that’s not going away it’s important you get it treated because acute pain can turn into chronic pain if not cared for.
The Impact Of Chronic Pain

A 2019 Deloitte report shows that:
- 1 in 5 Australians live with chronic pain.
- Over 3.2M Australians have chronic pain. That number is predicted to increase to 5.23M by 2050
- More than 1.8M Australians are limited in their activities due to chronic pain. It’s predicted to increase to 2.95M by 2050.
It’s also important to note that mental health disorders and chronic pain go hand in hand. It’s estimated that 45% of chronic pain patients also have anxiety or depression as a comorbidity. For more information about the impact of chronic pain on the Australian population you can visit the National Pain Week website.
Pain Treatments
There is a broad range of treatments for pain and chronic pain. The main, high level, categories of pain treatment would be surgical and non-surgical. When you look at non-surgical, categories are:
- Physical therapy
- Over the counter treatments
- Prescription pharmacological treatments
One of the better known pharmacological chronic pain treatments is opioids.
Opioids In Australia
It’s important to note that opioids are not all bad. They do have a place in treating chronic pain and other diseases. However, they are generally not a good long term pain treatment solution due to the addiction potential.
The Evolution of the Opioid Problem
Between the early ‘90s and the end of the first decade of this century we saw something like a two and a half thousand percent increase in the provision of prescription opioids to patients in Australia.
Over the last 30 years, there has been a shift in the medical fraternity to increase the use of opioids, by providing constant doses of opioids, to help provide around the clock pain relief for those with chronic pain. Unfortunately, by creating a constant blood level of opioids, the brain adapted to that level and asked for more.
Where once the vast majority of people having opioid overdoses would have been from heroin, we now see more than ¾ of overdoses from pharmaceutical opioids delivered on prescription.
Where once the vast majority of people presenting to the emergency department with an opioid overdose would have been from an injectable, illicit drug, such as heroin, we now see more than three quarters of them being the subject of therapeutic pharmaceutical opioids delivered on a prescription.
These people are not people the same people you think of as having a “drug habit” (to use a slang term), they are people who have been prescribed by a doctor and have developed a tolerance to that opioid and therefore require higher doses.
Opioids Are Surprisingly Addictive

Various studies in the US have demonstrated that, when a group of people are exposed to opioid treatment over a period of time, there is a certain percentage likelihood each month those people will become addicted.
It turns out that the number is about 30%. This doesn’t mean that these people will develop opioid use disorder. What it does mean is that regardless of their background, social circumstance and genetics, they will find it difficult to desist from treatment.
Prescription & Illicit Opioids Aren’t That Different
Whether an individual is taking an illicit opioid or a prescription, if an individual starts to show problematic use patterns, they develop the same three classic signs of addiction.
- Tolerance
- Withdrawal
- Salience (addictive drug seeking behaviours)
A Cycle Of Addiction
Many patients who are treated with opioids take them because they have arthritis or a bad back, or did when they began the drugs years ago.
With relation to individuals with chronic pain who have opioid use disorder, there is one other symptom that’s important to mention. This is the recurrence of the pain the individual thinks they’re treating by taking the opioid. Withdrawal from an opioid, classically causes back pain, leg pain, big muscle pain, bone, and joint pain.
So, when the opiate wears off, they get a rebound of back pain, big joint pain, big muscle pain, and they believe that their pain has recurred. So they need to take more of the drug.
Taking more of the drug increases their tolerance to the drug. But, taking more has less effect. Opioids also lend themselves to a condition where they change the brain’s appreciation or threshold for pain. This condition is called Opioid Induced Hyperalgesia. Opioid Induced Hyperalgesia is a condition where we see increasing amounts of opioid actually causing increasing baseline pain scores.
And so, the cycle begins again.
The Current State Of The Opioid Crisis
A study from 2018 showed that 56% of patients visiting a specialist pain clinic are taking opioid medications more than two days a week.
It’s estimated that about 3000 hospitalisations occurred for prescription opioid misuse and over 10,000 Australians received pharmacotherapy for prescription opioid misuse in 2017. As a result of this over 800 people died.
Not only is there a burden on human life, but there’s also a huge economic burden for individuals with chronic pain and the Australian community overall.
As mentioned, the type of individual being treated is no longer the heroin user that people often think about. Today these individuals may own their own home, have a university degree, a job in a multinational company, or run their own law firm. They may be a pharmacist, a doctor, a nurse, a nun or some other profession that has a pharmaceutical opioid problem and quite often have chronic pain.
So, the addiction case management principles and the goals that we’re looking for in treating these people are going to be different.
Treating Opioid Use Disorder
The traditional treatment of those with opioid use disorder is an opioid replacement therapy. Opioid replacement therapy is where doctors replace the opioid with another drug such as methadone or buprenorphine.
The drugs all do similar things, they occupy the opioid receptor, This means that the opioid the patient is used to absorbing, injecting or swallowing, doesn’t get a foot out in the brain. This does a few things:
- Reduces withdrawal and symptoms.
- Induces tolerance – the opioid no longer works when taken, reducing reward.
The problem for chronic pain patients is that it may not reduce their pain. It does for some people, but not for all. If the pain isn’t reduced then there’s still another major problem.
So, what are some potential solutions for this new problem? Cannabis could be the answer.
How Cannabis Is Helping
When it comes to treating chronic pain, cannabis is seen to be the new kid on the block. The funny fact is that cannabis has been used as a medicine for thousands of years. Most of what people know about the plant is likely untrue. Cannabis was given a bad name in the 1930s and became the outlaw drug it is today during the war on drugs in the 1970s.

When we talk about cannabis and chronic pain specifically there are two facts you should know:
- Cannabis has been proven to reduce pain in chronic pain patients by about 30%.
- About 70% of Australian medical cannabis access approvals are currently for chronic non-cancer pain.
As mentioned above, chronic pain often has a comorbidity of anxiety or depression. The second largest group of medical cannabis approvals is for mental health issues mainly anxiety, PTSD, and depression.
So, it would seem that cannabis has a place in the treatment of chronic pain.
Cannabis & Opioid Use Disorder
The research as quoted in the guidelines published in 2017 for chronic non-cancer pain indicate that medicinal cannabis has a moderate evidence level of reduction of pain by at least 30%.
Not only is there a pain score reduction, but some meta analyses indicate quite strongly that medicinal cannabis is opioid-sparing. This means that people can reduce their dose of opioids while they’re taking medicinal cannabis.
It turns out that if we keep patients on medicinal cannabis, they can stay off their opioids or at least stay on their opioids at a much lower dose. This has been my experience in clinical practice.
I’ve seen people who’ve taken opioids for pain relief for many, many years, sometimes at quite high doses have been able to taper.
And in most cases, desist from taking opioids completely whilst taking adequate doses of medicinal cannabis.
Research from the US also shows that opioid mortality rates drop when recreational cannabis becomes widely available via dispensaries. So, how exactly might cannabis be able to help with this problem?
Drug Liking, Lethality & Harm Reduction
The term “drug liking” has a colloquial meaning which is how much you like something, like it, love it etc. For people who are addicted to drugs, you can give them an opioid replacement therapy that doesn’t provide them with very much in the way of a feeling of liking or wellbeing.
The drug liking score for opioid replacement therapy amongst people who are takers of drugs is low. That’s very different from what you see with people who take a drug like a medicinal cannabinoid because they actually feel better on the drug than they did on their previous medications. It turns out that chronic pain sufferers may prefer cannabis over opioids. This in itself is improving their quality of life.
With any sort of drug use disorder, there’s a focus on harm reduction, particularly, preventing overdose.
The lethality of a medicinal cannabinoid is something like 1600 times less lethal than an opioid.
This number has been generated from a combination of animal and human studies.There are no recorded cases of an individual dying solely from cannabis. And, the recorded side effects of cannabis are fairly mild.
So, if the goals are:
- Prevent overdose
- Improve patient health and welfare
- Provide a framework of wellness
Then, due to cannabis’s harm reduction properties, it seems like cannabis could be the right choice.
If you replace someone who’s taking an opioid, who may be taking a tranquilliser to help them sleep at night, and maybe knocking off a few drinks at the bar and in the evening just to relax their back or the stress, the threshold for overdose is incredibly fine in that person.
If you take the opioid out, replace it with a cannabinoid, then the threshold for overdoses is incalculably huge. They’re not going to die of an overdose. They’re not going to have a respiratory depression episode. And my job as an addiction specialist is basically my first job is basically done.
I’ve prevented overdose and I’ve prevented some of the significant harms of their substance use.
It seems like cannabis may be able to help treat opioid addiction in the future.
What Needs To Change?

People won’t stop using opioids for pain unless they have something better to go to. Equally, doctors won’t stop prescribing opioids unless they’ve got something better to prescribe to their patients.
In Canada, we’ve seen medicinal cannabis go from a fourth line treatment to a second line treatment. In Australia, opioids are still considered as second line treatment as written in the TGA new guidelines. While pack sizes have been reduced and there are further restrictions on the provision of opioids for patients on the PBS, it’s still described as a second line treatment.
Is second line really the right answer for opioids, given their track record and their history over the last 20 years. And the answer is probably not.
Medicinal cannabinoids still require a Special Access Scheme approval through the TGA to be prescribed. They’re not seen as a second line treatment. Individuals who have a registration with the TGA are very few and far between. In many cases, medication for those with chronic disease are very expensive and there’s no support from the PBS.
So it begs the question, “How are we going to fund the newer more interesting or novel pain-relieving treatments that may have a less addictive potential, or if they do have addictive potential, have a less lethal potential versus all the more traditional pain medicines, which are still funded on the PBS.”
Opioids are still available to pensions and healthcare account holders for $6 a pack.
Again, this raises a question for clinicians and legislators.
Are we going to make an impact on this by just changing the price or the degree of red tape that a doctor has to go through in order to continue to prescribe opioids to patients? Or, are we going to do something else where we look beyond opioids to other treatments that may be able to reduce pain in patients?
What do you think?
We’d love to hear your opinions on chronic pain, the opioid crisis and medical cannabis. If you’d like to weigh in, please use the comment feature below or message us using the contact form.
If you know someone with chronic pain then we encourage you to reach out to them and make sure they know you’re there for them. If their current treatment isn’t working for them, perhaps cannabis can help.
Treating Chronic Pain: Opioids or Cannabis infographic